Individuals respond differently based on their own unique physiology.
As such, efforts are made to tailor treatments suited to your needs, belief systems, lifestyle, and any coexistent conditions and/or medications.
Heart Failure Management
Cardiac Catheterization
Coronary Angioplasty
Echocardiography
Stress Testing
What Is Heart Failure?
Heart failure is a condition in which the heart can't pump enough blood to meet the body's needs. In some cases, the heart can't fill with enough blood. In other cases, the heart can't pump blood to the rest of the body with enough force. Some people have both problems.
The term "heart failure" doesn't mean that your heart has stopped or is about to stop working. However, heart failure is a serious condition that requires medical care.
Overview
Heart failure develops over time as the heart's pumping action grows weaker. The condition can affect the right side of the heart only, or it can affect both sides of the heart. Most cases involve both sides of the heart.
Right-side heart failure occurs if the heart can't pump enough blood to the lungs to pick up oxygen. Left-side heart failure occurs if the heart can't pump enough oxygen-rich blood to the rest of the body.
Right-side heart failure may cause fluid to build up in the feet, ankles, legs, liver, abdomen, and the veins in the neck. Right-side and left-side heart failure also may cause shortness of breath and fatigue (tiredness).
The leading causes of heart failure are diseases that damage the heart. Examples include coronary heart disease (CHD), high blood pressure, and diabetes
Outlook
Heart failure is a very common condition. About 5.8 million people in the United States have heart failure.
Both children and adults can have the condition, although the symptoms and treatments differ. This article focuses on heart failure in adults.
Currently, heart failure has no cure. However, treatments—such as medicines and lifestyle changes—can help people who have the condition live longer and more active lives. Researchers continue to study new ways to treat heart failure and its complications.
For more information, please visit http://www.nhlbi.nih.gov/health/health-topics/topics/hf/
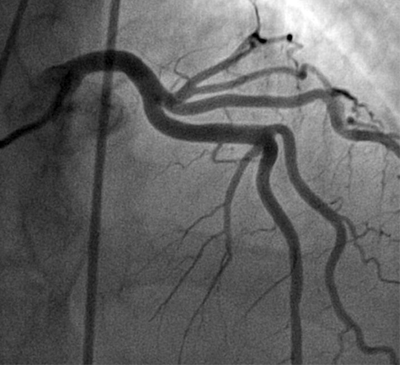
What Is Cardiac Catheterization?
Cardiac catheterization (KATH-eh-ter-ih-ZA-shun) is a medical procedure used to diagnose and treat some heart conditions.
A long, thin, flexible tube called a catheter is put into a blood vessel in your arm, groin (upper thigh), or neck and threaded to your heart. Through the catheter, your doctor can do diagnostic tests and treatments on your heart.
For example, your doctor may put a special type of dye in the catheter. The dye will flow through your bloodstream to your heart. Then, your doctor will take x-ray pictures of your heart. The dye will make your coronary (heart) arteries visible on the pictures. This test is called coronary angiography (an-jee-OG-rah-fee).
The dye can show whether a waxy substance called plaque (plak) has built up inside your coronary arteries. Plaque can narrow or block the arteries and restrict blood flow to your heart.
The buildup of plaque in the coronary arteries is called coronary heart disease (CHD) or coronary artery disease.
Doctors also can use ultrasound during cardiac catheterization to see blockages in the coronary arteries. Ultrasound uses sound waves to create detailed pictures of the heart's blood vessels.
Doctors may take samples of blood and heart muscle during cardiac catheterization or do minor heart surgery.
Cardiologists (heart specialists) usually do cardiac catheterization in a hospital. You're awake during the procedure, and it causes little or no pain. However, you may feel some soreness in the blood vessel where the catheter was inserted.
Cardiac catheterization rarely causes serious complications.
For more information, please visit http://www.nhlbi.nih.gov/health/health-topics/topics/cath/

What Is Coronary Angioplasty?
Coronary angioplasty (AN-jee-oh-plas-tee) is a procedure used to open narrow or blocked coronary (heart) arteries. The procedure restores blood flow to the heart muscle.
Overview
As you age, a waxy substance called plaque (plak) can build up inside your arteries. This condition is called atherosclerosis (ath-er-o-skler-O-sis).
Atherosclerosis can affect any artery in the body. When atherosclerosis affects the coronary arteries, the condition is called coronary heart disease (CHD) or coronary artery disease.
Over time, plaque can harden or rupture (break open). Hardened plaque narrows the coronary arteries and reduces the flow of oxygen-rich blood to the heart. This can cause chest pain or discomfort called angina (an-JI-nuh or AN-juh-nuh).
If the plaque ruptures, a blood clot can form on its surface. A large blood clot can mostly or completely block blood flow through a coronary artery. This is the most common cause of a heart attack. Over time, ruptured plaque also hardens and narrows the coronary arteries.
Angioplasty can restore blood flow to the heart. During the procedure, a thin, flexible catheter (tube) with a balloon at its tip is threaded through a blood vessel to the affected artery. Once in place, the balloon is inflated to compress the plaque against the artery wall. This restores blood flow through the artery.
Doctors may use the procedure to improve symptoms of CHD, such as angina. The procedure also can reduce heart muscle damage caused by a heart attack.
Outlook
Serious complications from angioplasty don't occur often. However, they can happen no matter how careful your doctor is or how well he or she does the procedure. The most common complications are discomfort and bleeding at the catheter insertion site.
Research on angioplasty is ongoing to make it safer and more effective and to prevent treated arteries from narrowing again.
For more information, please visit http://www.nhlbi.nih.gov/health/health-topics/topics/angioplasty/
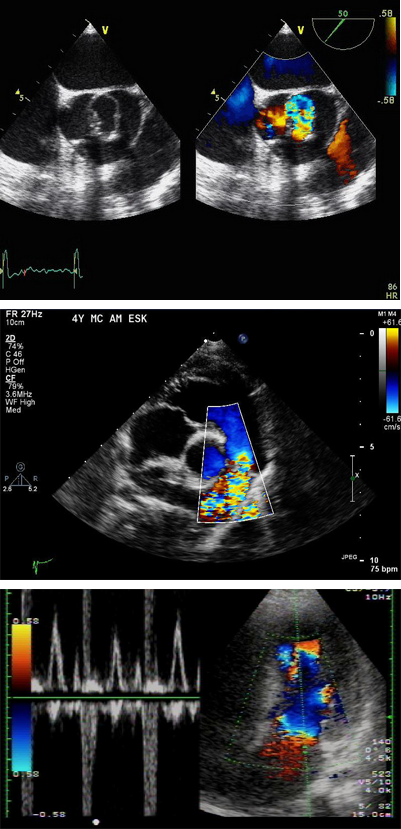
What Is Echocardiography?
Echocardiography (EK-o-kar-de-OG-rah-fee), or echo, is a painless test that uses sound waves to create moving pictures of your heart. The pictures show the size and shape of your heart. They also show how well your heart's chambers and valves are working.
Echo also can pinpoint areas of heart muscle that aren't contracting well because of poor blood flow or injury from a previous heart attack. A type of echo called Doppler ultrasound shows how well blood flows through your heart's chambers and valves.
Echo can detect possible blood clots inside the heart, fluid buildup in the pericardium (the sac around the heart), and problems with the aorta. The aorta is the main artery that carries oxygen-rich blood from your heart to your body.
Doctors also use echo to detect heart problems in infants and children.
For more information, please visit http://www.nhlbi.nih.gov/health/health-topics/topics/echo/
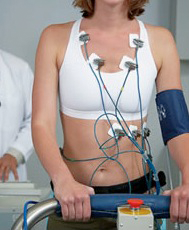
What Is Stress Testing?
Stress testing provides information about how your heart works during physical stress. Some heart problems are easier to diagnose when your heart is working hard and beating fast.
During stress testing, you exercise (walk or run on a treadmill or pedal a stationary bike) to make your heart work hard and beat fast. Tests are done on your heart while you exercise.
You might have arthritis or another medical problem that prevents you from exercising during a stress test. If so, your doctor may give you medicine to make your heart work hard, as it would during exercise. This is called a pharmacological (FAR-ma-ko-LOJ-ih-kal) stress test.
Overview
Doctors usually use stress testing to help diagnose coronary heart disease (CHD). They also use stress testing to find out the severity of CHD.
CHD is a disease in which a waxy substance called plaque (plak) builds up in the coronary arteries. These arteries supply oxygen-rich blood to your heart.
Plaque narrows the arteries and reduces blood flow to your heart muscle. The buildup of plaque also makes it more likely that blood clots will form in your arteries. Blood clots can mostly or completely block blood flow through an artery. This can lead to chest pain called angina (an-JI-nuh or AN-juh-nuh) or a heart attack.
You may not have any signs or symptoms of CHD when your heart is at rest. But when your heart has to work harder during exercise, it needs more blood and oxygen. Narrow arteries can't supply enough blood for your heart to work well. As a result, signs and symptoms of CHD may occur only during exercise.
A stress test can detect the following problems, which may suggest that your heart isn't getting enough blood during exercise:
• Abnormal changes in your heart rate or blood pressure
• Symptoms such as shortness of breath or chest pain, especially if they occur at low levels of exercise
• Abnormal changes in your heart's rhythm or electrical activity
During a stress test, if you can't exercise for as long as what is considered normal for someone your age, it may be a sign that not enough blood is flowing to your heart. However, other factors besides CHD can prevent you from exercising long enough (for example, lung disease, anemia, or poor general fitness).
Doctors also may use stress testing to assess other problems, such as heart valve disease or heart failure.
For more information, please visit http://www.nhlbi.nih.gov/health/health-topics/topics/stress/
SITE DESIGN & DEVELOPMENT BY EYE ENGINE
©2014 LAKHANI CARDIOLOGY. ALL RIGHTS RESERVED.
2925 North Sycamore Drive, Suite 310
Simi Valley, CA 93065
T (805) 527-2570
F (805) 527-2978
Office Hours:
Monday - Friday
8:30 a.m. - 5:00 p.m.
Saturday (appointment only)
Closed Sunday
Home Visits:
By appointment only,
based on availability
We accept most PPO insurance plans
(please call our office to verify), Medicare, cash, and credit card payments
